Laser Gum Surgery
Dr. Hamed H. Javadai of Marin Reconstructive Periodontics utilizes the newest in Waterlase MD, which is a revolutionary dental device that uses a combination of laser energy and water to perform many traditional dental procedures without anesthesia or pain.
The Waterlase MD, uses a less invasive approach that conserves healthy tooth structure, which helps teeth function better and last longer.
Laser Surgery with Waterlase
The Waterlase MD is a revolutionary dental device that uses a combination of laser energy and water to perform many traditional dental procedures without anesthesia or pain. The Waterlase MD, uses a less invasive approach that conserves healthy tooth structure, which helps teeth function better and last longer.
When the traditional dental drill is used, heat and vibration are the major causes of most of the pain. The Waterlase MD works so fast and avoids both heat and vibration, so the tooth nerve can't respond to register pain. This means no shots or the numb feeling after the dental visit.
The Waterlase MD can also perform many soft tissue or gum procedures with little or no discomfort or bleeding.

Bone Grafting
Bone grafting is commonly performed by an oral and maxillofacial surgeon to replace or augment bone in areas of tooth loss. Bone grafting to the jaws and facial structures may be necessary in a wide variety of scenarios. The most common bone grafts are facial skeleton and jaw procedures. Other common procedures include tooth extraction site graft, bone graft reconstruction and for a sinus lift. Shrinkage of bone often occurs when a tooth is lost due to trauma, severe caries, or periodontal disease. Additionally, bone loss may have already occurred due to infection or pathology around a tooth. There are many artificial biocompatible bone substitutes available; however, the best material for a bone graft is your own bone, which most likely will come from your chin, the back part of your lower jaw or your hip bone. The hip is considered to be a better source because the hip bone has a lot of marrow, which contains bone-forming cells. There are also synthetic materials that can be used for bone grafting. Most bone grafts use a person's own bone, possibly in combination with other materials.
To place the removed bone in the recipient site, little holes are drilled in the existing bone to cause bleeding. This is done because blood provides cells that help the bone heal. The block of bone that was removed will be anchored in place with titanium screws. A mixture of the patient's bone marrow and some other bone-graft material will then be placed around the edges of bone block. Finally, a membrane is placed over the area and the incision closed.
The bone graft will take about 6 to 12 months to heal before dental implants can be placed. At that time, the titanium screws used to anchor the bone block in place will be removed before the implant is placed.
Tooth Extraction
When the extraction of a tooth is required:
- An incision in the gums is made
- The tooth is removed
- The area is stitched up and is allowed to heal
During this time, it is important to think about a tooth replacement option. An extracted tooth leaves an open area in the jaw which, in time, allows the neighboring teeth to drift into the area where the tooth was extracted. This in turn, causes a chain reaction to all the surrounding teeth. Also, if you are considering placing an implant in the future, you should consider asking your dentist to place a bone graft at the time of surgery to preserve the bone width and height.
Wisdom Tooth Problems
The problems involving your wisdom teeth may be caused by the size of your jaw and/or by how crowded your teeth are. Common warning symptoms that there is an un-natural problem in the development of your wisdom teeth could be pain and swelling.
Symptoms can be caused by:
- Infection to the gums
- A crowded tooth displacing neighboring teeth
- A decayed wisdom tooth
- Poorly positioned wisdom tooth
- A cyst that destroys bone
Oral Pathology
The inside of the mouth is normally lined with a special type of skin (mucosa) that is smooth and coral pink in color. Any alteration in this appearance could be a warning sign for a pathological process. The most serious of these is oral cancer. The following can be signs at the beginning of a pathologic process or cancerous growth:
The following can be signs at the beginning of a pathologic process or cancerous growth:
- Reddish patches (erythroplasia) or whitish patches (leukoplakia) in the mouth.
- A sore that fails to heal and bleeds easily.
- A lump or thickening on the skin lining the inside of the mouth.
- Chronic sore throat or hoarseness.
- Difficulty in chewing or swallowing.
These changes can be detected on the lips, cheeks, palate and gum tissue around the teeth, tongue, face and/or neck. Pain does not always occur with pathology, and curiously, is not often associated with oral cancer. However, any patient with facial and/or oral pain without an obvious cause or reason may also be at risk for oral cancer.
Ankylosis
This refers to a tooth or teeth (primary or permanent) that have become "fused" to the bone, preventing it or them from moving "down" with the bone as the jaws grow. This process can affect any teeth in the mouth, but it is more common on primary first molars and teeth that have suffered trauma (typically the incisors). Treatment can vary depending on the degree of severity of the ankylosis (how "sunken into the gums" a tooth may appear). The degree of severity usually will vary depending on how early the process started, and as a general rule, the earlier it starts, the more severe the ankylosis becomes with age. Several considerations must be taken before any treatment is provided, and your dentist will discuss all the risks and benefits of each treatment option.

Crown Lengthening
Crown lengthening is a surgical procedure that re-contours the gum tissue and often the underlying bone of a tooth. Crown lengthening is often for a tooth to be fitted with a crown. It provides necessary space between the supporting bone and crown, which prevents the new crown from damaging bone and gum tissue.
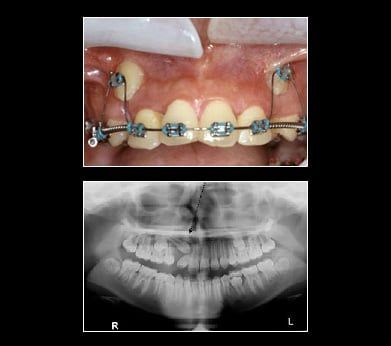
Impacted Canine
Impacted canines may be retrieved with braces, using a surgical approach via a gold chain or straight wire. Tissue covering the tooth is uncovered. A chain or wire is attached to the tooth crown. Tissue is placed back over the tooth leaving the chain or wire coming out of the gum. For the purpose of this illustration a gold chain is used to retrieve the canines. The chain is attached to the tooth crown and the link is attached to a flexible archwire so that the wire is active (bent). Once a month, the wire is reactivated by using the next link up on the chain until the impacted canine erupts enough to attach a regular bracket on the canine. With the regular bracket in place, a more flexible wire is added directly to the bracketed canine. This process will bring the canine into position within the arch by forcing the canine to conform to the straight archwire form. This is a long process taking anywhere from 8-12 months.
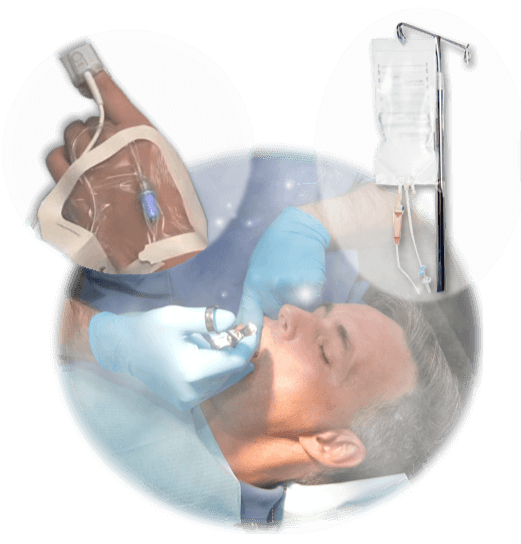
Sedation Dentistry
Sedation dentistry administers medication to help dental patients remain calm and relaxed prior to and during dental procedures. If you are experiencing an uncomfortably high level of anxiety, Dr. Javadi may recommend dental sedation. The most common form of dental sedation is an oral medication or nitrous oxide gas which is inhaled.
Decades of research and successful practice have shown that the inhalation of a mix of nitrous oxide and oxygen provides fast, effective analgesia, pain relief and, relaxation. Allowing Dr. Javadi to complete your dental work while you stay absolutely comfortable. Nitrous oxide takes effect almost instantly and is out of the patient's system within a few minutes, allowing a patient to quickly return to normal activities after dental work is complete.
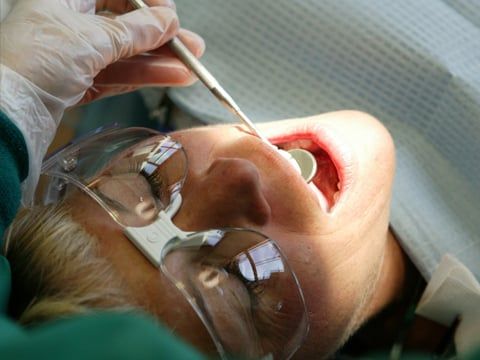
Sedation Dentistry: The use of Laughing Gas & Oxygen for Sedation
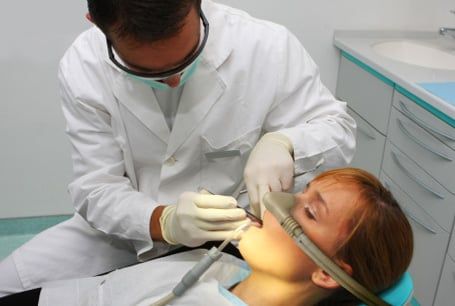
The calming inhalant known as laughing gas is for patients who are mildly or moderately anxious or nervous. It eases their anxieties so that they can relax and undergo treatment comfortably and safely. The gas is administered by placing a small hood over the patient's nose. As the gas takes effect, the patient becomes relaxed, but is still awake and can communicate. When the gas is turned off, the effects of sedation wear off almost immediately.
Sedation FAQs
What is the medication?:
One of many safe and widely-used sleeping pills will be used. In certain cases, nitrous oxide gas may also be used as an additional medication.
Can I drive home?:
No. The effects last many hours and driving is not safe. We will call your ride at the end of your appointment to bring you home. You should not plan to do anything but sleep for the rest of the day. By the next morning you will feel normal, rested and ready to get on with your life.
Will you use local anesthetic (Novocain)?:
Always. Oral sedation is not general anesthesia. Treatment is no different than if you were not sedated. The difference is that you will be much more relaxed, memory of the procedure will be minimal and the time will seem to fly by.
Will I be asleep?:
Most people do doze during their appointment, but our primary goal is relaxation and comfort with safety.
How safe is it?:
Properly administered oral sedation is the safest form of sedation. We use sophisticated monitoring equipment during all procedures and you are always attended by a trained doctor or staff member.
Is it expensive?:
No. There is a sedation fee to cover the expense of the drugs and the monitoring, but we don't try to profit from sedation. Our profit (and yours) is in your comfort and in the quality of your care.
Would I be unusual in wanting sedation?:
Not at all. Oral sedation in our office is very popular for surgery, for long appointments and for complicated procedures as well as for basic dental anxiety.
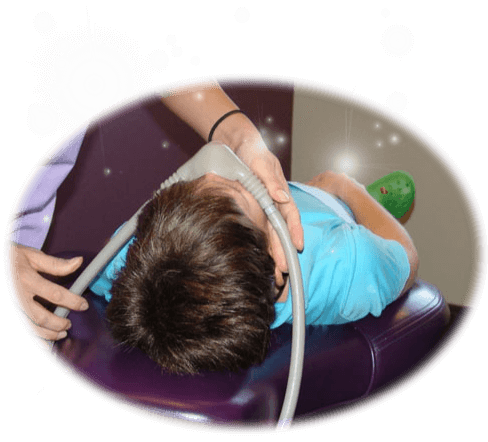
Oral Sedation
Patients who are more anxious may need an oral medication that is stronger than nitrous oxide. With oral sedation, the patient may be sleepy but can be aroused if necessary and can respond to simple commands.
Minor side effects such as nausea or vomiting can occur with some medications. Before a visit in which a patient is to receive oral sedation, he/she should receive instructions about eating and drinking, what to expect and what to watch for after treatment. You may need assistance to get home after sedation. Patients may need to stay for a short observation after dental treatment has been completed.

IV Sedation
Injection or intravenous (into a vein) methods require more experience to be administered and monitored properly. Injections and intravenous medications should be used only by dentists with extensive training in these techniques.
General anesthesia puts a patient into a deep sleep. He or she is unable to feel pain or to move around. General anesthesia may be recommended if the patient:
- Can't relax or calm down enough for treatment to be performed safely, even with conscious sedation and other behavior management techniques
- Needs oral surgery or other dental treatment that would be difficult for the patient to tolerate while awake
- Needs a lot of dental work that can best be done in one long appointment rather than many shorter visits
- Has a medical, physical or emotional disability that limits his or her ability to understand directions and be treated safely as an outpatient
Some general dentists have received training and a certification in general anesthesia, while others contract with an anesthesiologist. These professionals are trained to deliver the medications and monitor patients during the procedure and handle any complications that may occur.